A research group at the University of Calgary has watched the binding of fluorescent Borrelia
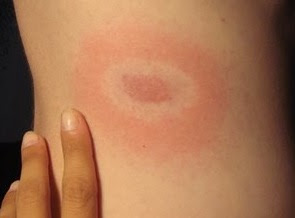 burgdorferi spirochetes, the Lyme disease pathogen, to the surface of blood vessels in mice. (ref. below) A small heparin molecule was shown to block this interaction between the spirochete surface protein BBK32 and the heparan sulfate proteoglycans of the endothelial cells of the skin blood vessels.
burgdorferi spirochetes, the Lyme disease pathogen, to the surface of blood vessels in mice. (ref. below) A small heparin molecule was shown to block this interaction between the spirochete surface protein BBK32 and the heparan sulfate proteoglycans of the endothelial cells of the skin blood vessels.The heparin-binding domains in the spirochete protein, BBK32 are easy to spot in the amino acid sequence of this protein that I downloaded from the NCBI protein database:
>gi|19072701|gb|AAL84596.1| BBK32 [Borrelia burgdorferi]
MKKVKSKYLALGLLFGFISCDLFIRYEMKEESPGLFDKGNSILET
SEESIKKPMNKKGKKIARKKGKSKVSRKEPYIHSLKRDSANKSN
FLQKNVILEEESLKTELLKEQSETRKEKIQKQQDEYKGMTQGSL
NSLSGESGELKETIESNEIDITIDSDLRPKSSLQDIAGSNSISYTDE
IEEEDYARYYLDEDDEDDEYYEDDYEEIRLSNRYQSYLEGVKYNV
DSAINTINKIYDTYTLFSTKLTQMYSTRLDNLAKAKAKEEAAKFTK
EDLEKNFKTLLNYIQVSVKTAANFVYINDTHAKRKLENIEAEIKTL
IAKIKEQSNLYEAYKAIVTSILLMRDSLKEVQGIIDKNGVWY
Basic amino acids are K=lysine, R=arginine
The minimal heparin binding pairs, e.g. KKVKSK are shown in red and the strong heparin-binding triplets, e.g. KRK, are shown in blue. Notice that one triplet is augmented with several pairs to further enhance heparin binding.
I would also expect that BBK32 would be internalized into host cells and transported into the nucleus, where it may alter transcription, a la HIV-TAT. The existence of multiple, strong heparin-binding domains may also serve to bind the BBK32 (or the spirochetes) to multiple different heparan sulfate proteoglycans and interfere with the HSPG circulation system. This may have a toxic effect.
reference:
Norman MU, Moriarty TJ, Dresser AR, Millen B, Kubes P, Chaconas G. Molecular mechanisms involved in vascular interactions of the Lyme disease pathogen in a living host. PLoS Pathog. 2008 Oct 3;4(10):e1000169.

17 comments:
Interesting. Do you know if any one has tried heparin as a treatment for Lyme Disease or any other disease which relies on heparin binding domains?
The list of viruses and bacteria that use surface heparan sulfate proteoglycans to gain entry into human cells is very long. It includes HIV, flu, E. coli, etc. Heparin is routinely used by the lungs and gut, where it is actively secreted by mast cells (along with histamine and proteases). After all, pharmaceutical heparin is produced from cattle and pig lungs and intestines. So heparin is routinely used by the body to reduce infections.
The question is why we get sick if our immune system is producing heparin to give our cells a protective coating? The answer is in two parts -- the body uses heparan sulfates for signaling and heparin (fragments of heparan sulfate) is used to control inflammation.
Adding extra heparin effects hundreds of protein systems and can potentially disrupt systems, such as blood clotting. Heparin is also quick circulated and metabolized cells -- half life for heparan sulfate proteoglycans is six hours.
Inflammation reduces heparan sulfate proteoglycan production. Since HSPG is the major barrier to proteins in the basement membranes, inflammatory reduction in HSPG results in loss of proteins into the urine in kidneys, makes the gut leaky and makes the blood brain barrier leaky. Added heparin can repair these leaks, but it is temporary.
The simple answer to your question is that heparin should be useful to wash away a pathogen, but in a situation such as a tick bite, immediate, local penetrating sterilization might be more effective. I wouldn't expect heparin to provide systemic protection, it would be more likely to enhance spread.
This is complex and poorly understood.
Thanks for your comment.
Art
Explanations such as this are very helpful for interested readers who are not molecular biologists.
I was expecting the conclusion to be that systemic inflammation could be an aggravating factor in becoming infected by the spirochete. Perhaps that conclusion would be too speculative with what is known at this time.
This topic is of great interest to me since the black legged tick is moving into the area and I spend a great deal of time outdoors.
William,
The spirochetes are very dangerous and have a tendency to spread to the nervous system and produce chronic cryptic infections with neurological complications. They just haven't received enough research attention and are much more common than the public accepts. The ticks also inject numerous other bacteria, to further complicate symptoms and treatment.
In tick country (I guess anywhere, since the presence of ticks is frequently not known) it pays to be very vigilant and knowledgeable.
Chronic inflammation could contribute to the course of the infection and response to antibiotics. Little is known.
Thanks for your comments.
(I'm not sure where to put this note but here seems as good as anywhere. Let me know if you feel it is too far off topic.)
I picked up some "chigger bites" last weekend and decided to use some of the information on this blog to do some experiments.
Chiggers are the larval form of a mite and they feed on animal skin. The larvae are very small but they inject a substance dissolves the tissue, which then lap up. Even tho the wound is small a red, inflamed and intensely itchy area develops. For me anyway, these areas get worse for a week and then get better for a week and then they are gone. They are an annoyance so are not a big deal.
Since an inflammation occurs I decided to try castor oil & Vicks on a couple of the areas to see if that would help. I put some of these two materials on two band-aids and left them on for a day.
At the end of the day, the area under the castor oil bandage was less red and less itchy but the next day it was back to full redness. The area under the vicks bandage was quite a bit less red and didn't itch at all the next day.
This one experiment is not very conclusive since sometimes a "bite" will start off strong and then suddenly wither away to nothing all on its own. I'll definitely try it again the next time I get some of these bites and get a better idea of the worth of these treatments.
William,
Those are interesting results. The castor oil will act as an anti-inflammatory, but I wouldn't expect it to be very toxic to those nasty larvae (I had the same experience when I lived in Missouri.) The Vicks VapoRub is a combination of antimicrobials that should also be toxic to the larvae and anti-inflammatories. So it makes sense that both will temporarily reduce inflammation, but the Vicks will kill the larvae and suppress inflammation.
Vicks is great. I even reached for a tub of Vicks when I grabbed a hot pan in the kitchen. I quickly applied it to my wrist and the pain was gone in half a minute and I didn't notice it the next day. I was pleased that I reacted on my beliefs and it paid off. Without the Vicks, I would have had blisters.
Thanks for the comments.
I tried another castor oil experiment with poor results.
This time I got a small patch of poison ivy dermatitis on my forearm from pulling up some poison ivy vines while wearing only gloves and a short sleeve shirt. I'm not very allergic so I had only a small spot, about 1 cm^2. As with chigger bites, my typical reaction is for it to get worse for a week then better for an week and then it's gone.
I didn't do anything for a few days and then remembered that it might be interesting to try a topical inflammation reducer. So, the next morning I put a small amount of castor oil on a bandaid and put it over the dermatitis. During the day the itching became worse and when I took the bandaid off at the end of the day the dermatitis was redder than in the morning.
It remained itchy for the next few days but eventually the whole irritated area went away after two weeks, just like usual. Next time I'll try some Vicks but I don't expect it to work any better.
William,
I would have expected that result. The castor oil would be a good solvent for the poison ivy irritant and spread it.
I think that you would have had a better result by washing the area with soap and plenty of water. The castor oil or VicksVaporub could have been applied outside of the area already inflamed. In this way the heat or cold sensing nerves that detect the chemicals could trigger an opiod response via the vagus nerve to the general area and reduce inflammation. I would expect that application of castor oil to your elbow would have been effective.
Castor oil, capsaicin and menthol are not directly anti-inflammatory and don't bind to NFkB, for example, like aspirin.
castor oil also activates the lymphatic system - so besides spreading the poison ivy irritant due to it's solvent qualities, it also spreads it by moving it away from the area of containment through the lymph.
I was 23 Years old when diagnosed with a-fib for unknown reasons electro-cardioversion worked for a couple of months,suffer bouts of pneumonia/bronchitis,sweat profusely in cool climates,was diagnosed with osteoporosis/degenerative disk disorder. Although strong effort has been made on the part of my physician (for seperate conditions).My coumadin therapy is pretty high dose (15mg a day)without achieving therapeutic range .Does the spirochete associated with lyme disease thicken the blood? From what I can gather these spirochetes can prove elusive if not undetectable at certain stages of their life cycle is there a definitive test?i.e spinal tap
Anonymous,
It seems to me that all of your symptoms point to high levels of chronic inflammation. One of the consequences of high levels of inflammation is suppression of heparan sulfate proteoglycan production, which increases clotting and reduces blood barriers to the brain, kidney and gut. That makes you leaky.
The anti-inflammatory diet that I recommend should put a stop to the leakiness and should reduce the need for blood thinners. Look at the diet, get your blood vit.D level measured, adjust the vit. D with supplements, eliminate grains, reduce carbs, increase your saturated fats, eliminate vegetable oils, use olive oil/butter, eat plenty of meat/fish/eggs/dairy and veggies. Then work on your gut with probiotics and soluble fiber (pectin, inulin in apples and leeks.) You should see dramatic results in 2-4 weeks.
I don't know why you are mentioning Lyme, but the general approach recommended should help. Let me know if you observe paradoxical responses, e.g. aching of joints.
Thanks for the questions.
شركة مكافحة السحالي بالرياض
شركة مكافحة الجنادب بالرياض
شركة مكافحة المن بالرياض
شركة مكافحة الديدان بالرياض
شركة مكافحة الباعوض بالرياض
شركة مكافحة الحيات بالرياض
شركة مكافحة اليراسيع بالرياض
شركة مكافحة الجراد بالرياض
شركة مكافحة العنكبوت بالرياض
شركة مكافحة الدبور بالرياض
شركة مكافحة السناجب بالرياض
شركة مكافحة النمل الاسود بالرياض
شركة تنظيف مكاتب بالرياض
I am glad to see this site share valued information Nice one! Great dayyy... MM
I have to thank you for the efforts in this blog. the quality is good thanks... MM
Really amazed with your writing talent. Thanks for sharing, Love your works... MM
Fantastic website. A lot of helpful info here. Thanks to the effort you put... MM
Extremely pleasant and fascinating post. Continue posting. We're waiting Thanks... MM
Post a Comment